Selective internal radiation therapy (SIRT)
SIRT provides treatment for liver tumours by direct delivery of radioactive microscopic beads (SIR-Spheres) to the tumour site(s). SIR-Spheres® release radiation energy called “Beta” radiation; a common type of radiation also used in other nuclear medicine therapy.
SIRT provides treatment for liver tumours by direct delivery of radioactive microscopic beads (SIR-Spheres) to the tumour site(s). SIR-Spheres® release radiation energy called “Beta” radiation; a common type of radiation also used in other nuclear medicine therapy.
SIRT can be performed on tumours local to the liver ,or secondary tumours that have spread from other parts of the body to the liver.
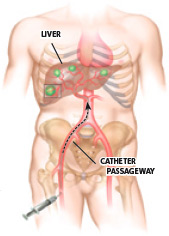
These tiny microspheres are lodged directly into the blood supply feeding these tumours, allowing the radiation to be delivered directly to the tumour.
The radiation given off by the beads extends to an area of about 4mm which means that there is little damage to healthy tissue in the liver and no significant level of radiation outside the body. The radioactivity of the beads decreases over time, with its treatment effect occuring mainly within the first two days. It is almost gone by day 11.
SIRT involves two separate procedures. The first procedure is the preparation or work-up stage. The second stage occurs two weeks later, where the delivery of SIR-Spheres® occurs.